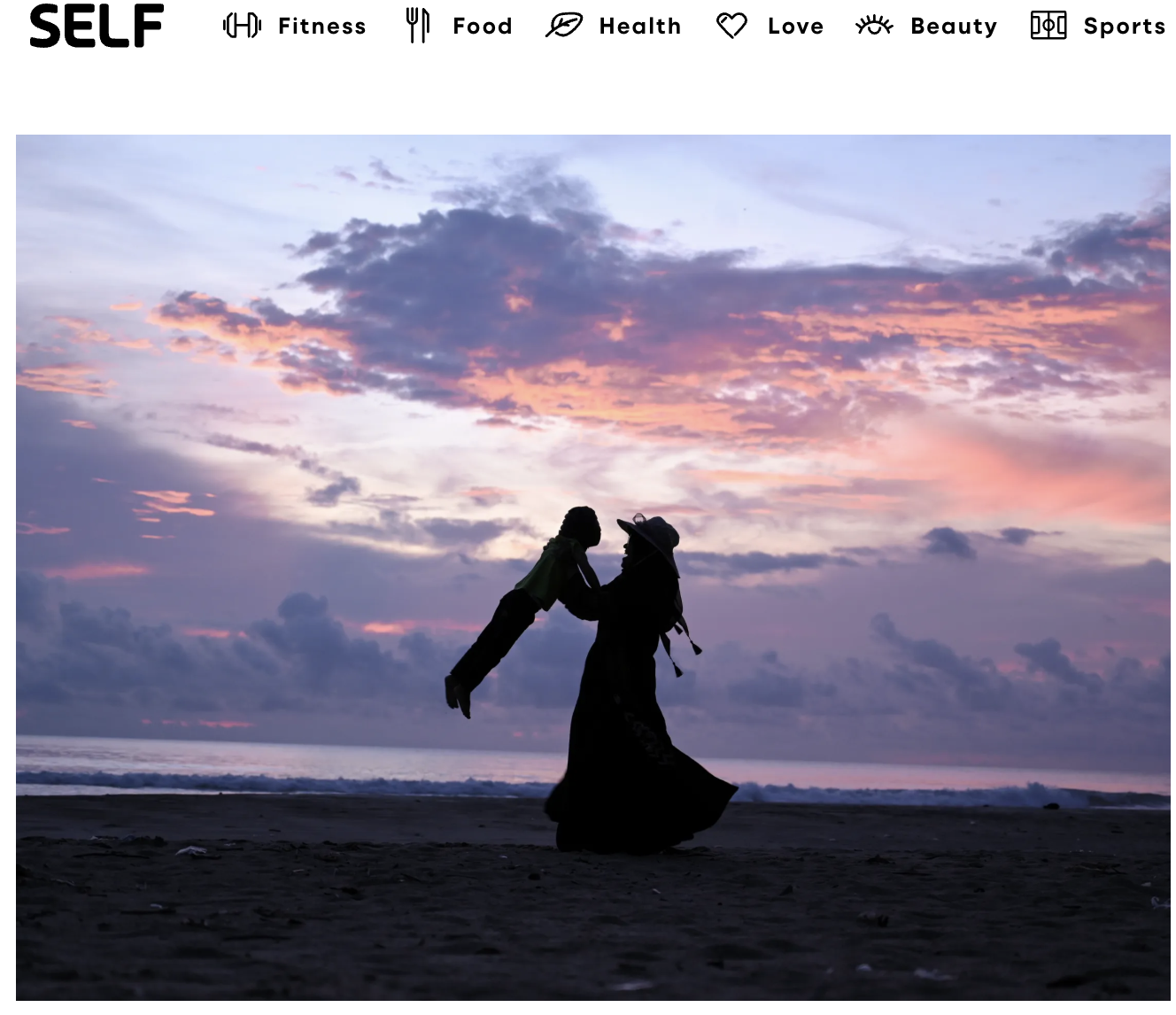
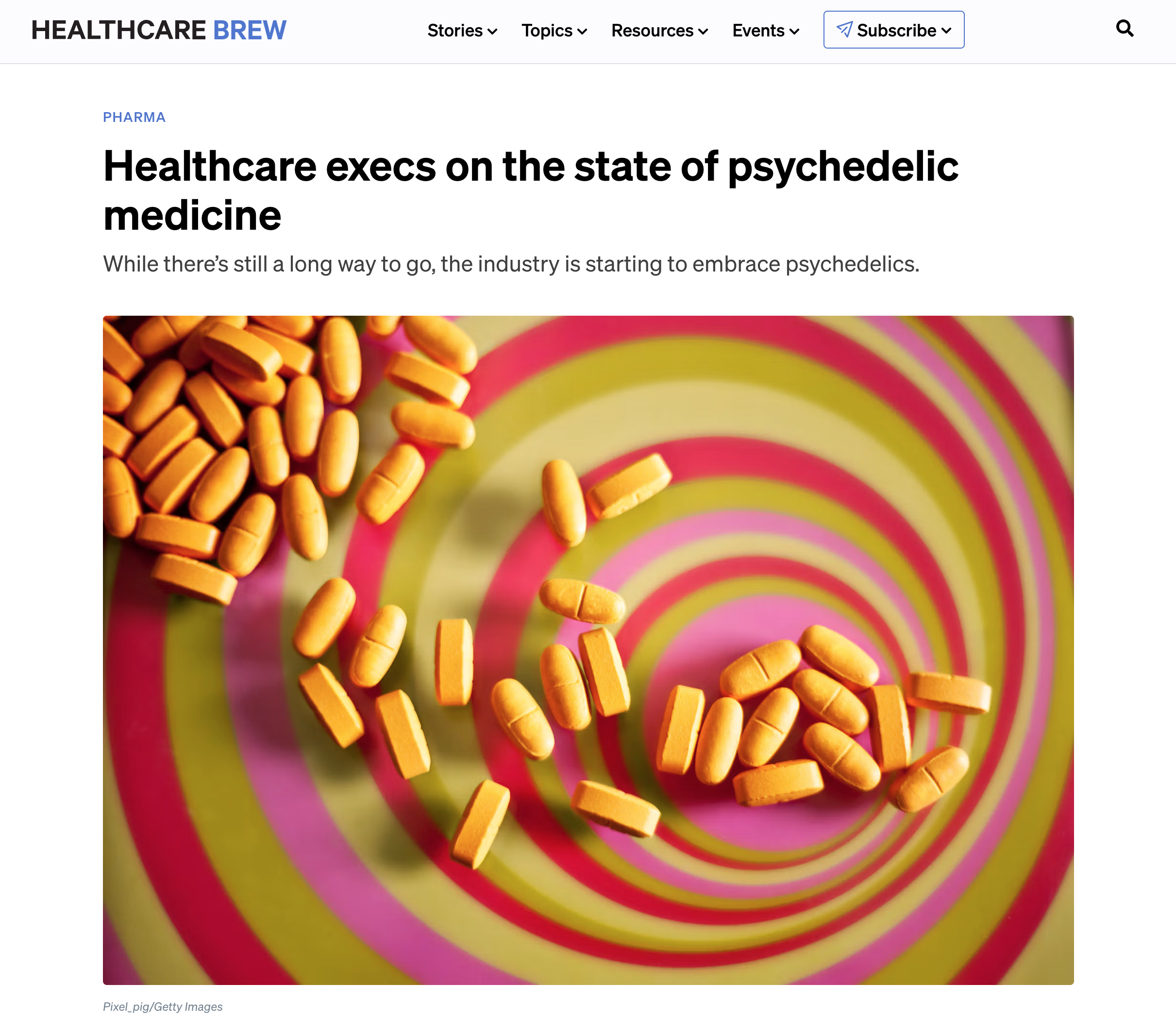
The Traumatic Stress Division and The Parsons Research Center for Psychedelic Healing at Icahn School of Medicine at Mount Sinai are at the forefront of research on trauma, PTSD, depression, and other mental health disparities. Founded by Dr. Rachel Yehuda in 2020, the Parsons Research Center builds on her 30-year career studying PTSD and the intergenerational effects of trauma. Her pioneering work through the Division of Traumatic Stress Studies laid the foundation for our current focus on innovative treatments like psychedelic-assisted therapy (PAT).
In collaboration with leading research centers and organizations, including Mount Sinai’s Depression and Anxiety Center and the Eating and Weight Disorders Program, and the VA Spinal Cord Injury Research Center, partnerships with psychedelic pharmaceutical companies, we employ a multidisciplinary approach to understanding and treating mental health conditions.
We invite individuals affected by trauma, depression, and other mental health conditions to participate in our clinical research trials to explore cutting-edge treatment options. Our research contributes to the evolving understanding of trauma, depression, and PTSD, advancing treatment options and expanding knowledge in the field.
A New Model for Treatment
While current treatments such as psychological therapies (e.g., exposure therapy) and pharmacological interventions (e.g., selective serotonin reuptake inhibitors, or SSRIs) provide relief for some, a significant portion of patients remain symptomatic, highlighting the need for novel approaches. Psychedelics are being studied for their potential to alleviate mental health symptoms due to their profound effects on brain function, cognition, and emotional regulation. By altering cognition, perception, and mood, these drugs can help reshape how the brain processes trauma and emotional distress, providing a promising avenue for treatment in individuals who have not found relief from traditional therapies.
Division of Traumatic Stress Studies
Our multidisciplinary research program explores the complex connections between trauma, epigenetics, and biology, focusing on how traumatic experiences shape both mind and body. We conduct groundbreaking studies in molecular biology, neuroscience, and epigenetics, with an emphasis on PTSD, resilience, and intergenerational trauma.
Our pioneering work includes investigating epigenetic mechanisms in populations such as the offspring of Holocaust survivors and children born to mothers exposed to the 9/11 attacks. We are also leading research in PTSD, utilizing cutting-edge technologies like stress-stimulated induced neurons to better understand how trauma impacts future generations.


Collaboration and Growth
In partnership with the VA and Mount Sinai, we’re advancing psychedelic research across leading labs and clinical centers to address mental health disparities– including depression, suicidality, bulimia, and intergenerational trauma. Our current research includes MDMA dose optimization studies with veterans with PTSD, psilocybin- and ketamine-assisted therapy trials with the Depression and Anxiety Center, psilocybin therapy for spinal cord injured veterans, psilocybin therapy for intergenerational trauma, and MDMA-assisted therapy for mental healthcare providers. A significant portion of this work takes place in our new, purpose-built space at 112th and Broadway, through Mount Sinai– designed to support innovative, trauma-informed care and groundbreaking clinical research.
For more information, please visit the The Parsons Research Center for Psychedelic Healing.